As a healthcare provider, I know that making the decision to move forward with a procedure for your child is never easy. Whether you have a newborn struggling to latch or a toddler dealing with speech delays, undergoing a frenectomy (often called a tongue-tie or lip-tie release) is a big step toward better health and function. However, as Dr. Sepehr Nassiripour, I often tell the parents in my practice that the procedure is only half the battle. The true success of the treatment relies heavily on what happens at home during the healing process.
I have written this comprehensive guide to walk you through everything you need to know. My goal is to make the tongue tie release recovery journey as smooth, stress-free, and successful as possible for both you and your little one.
Understanding the “Why” Behind the Recovery Process
Before we dive into the specific steps of aftercare, it is helpful to understand how the mouth heals. The mouth is an incredibly resilient environment. It heals faster than almost any other part of the body. While this is generally a good thing, it presents a unique challenge after a frenectomy.
Because the mouth heals so quickly, the tissues naturally want to close up and stick back together. If the two sides of the release site fuse prematurely, the tongue or lip can become tight again. This is known as re-attachment. The primary goal of the recovery stretches and exercises I prescribe is to keep those raw surfaces apart while they heal, ensuring the new range of motion is permanent.
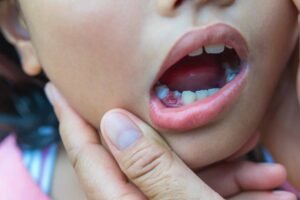
According to Stanford Medicine Children’s Health, tongue-tie (ankyloglossia) is a common condition that can restrict the tongue’s range of motion. By following a strict recovery protocol, we ensure that the surgical release leads to lasting functional improvement.
Immediate Aftermath: The First 24 Hours
The first day is often the hardest for parents emotionally. It is completely normal to feel nervous. Immediately following the procedure, your child may be numb if a local anesthetic was used. As this wears off, they might be fussy or frustrated.
Managing Discomfort
While the laser procedure causes minimal bleeding and seals nerve endings, there will be some soreness. Think of it like a “pizza burn”—that feeling when you bite into hot food and burn the roof of your mouth. It is annoying and sore, but it is manageable.
I generally recommend using age-appropriate pain relief, such as Tylenol (acetaminophen) or Motrin (ibuprofen), based on your child’s age and weight. Please always consult your pediatrician before administering medication. For a more natural approach, many parents find success with:
- Skin-to-skin contact: This releases oxytocin and calms the baby.
- Frozen breast milk chips: If your baby is old enough for solids or distinct textures, small slivers of frozen milk can numb the area naturally.
- Warm baths: A soothing bath can distract the baby and help them relax before bedtime.
The Critical Component: Active Wound Management (Stretches)
This is the part that makes most parents nervous, but I promise you, you can do this. To prevent the tongue tie release recovery from failing due to re-attachment, you must perform stretches. I usually recommend doing these stretches 4 to 6 times a day for the first three weeks, but always follow the specific instructions I give you during our appointment.
How to Perform the Tongue Stretch
The goal is to visualize a diamond shape at the wound site. Here is the technique I recommend:
- Wash your hands thoroughly. You can use non-latex gloves if you prefer, but clean fingers work well.
- Place the baby on a flat surface, like a changing table or a bed. It is often easiest to approach them from behind their head (so you are looking upside down into their mouth).
- Place your two index fingers under the tongue. You want to get deep, aiming for the “floor” of the mouth, not just the tip of the tongue.
- Gently but firmly lift the tongue up and back towards the throat. You are trying to stretch the diamond wound vertically.
- Hold this position for a few seconds. You want to see the diamond shape open up completely.
How to Perform the Lip Stretch
If your child also had a lip-tie released, you will need to stretch that area too.
- Place your index fingers at the very top of the gum line, deep in the fold of the lip.
- Lift the lip up and back toward the nose.
- Ideally, you want the lip to cover the nostrils gently. This ensures the raw surfaces of the lip and the gum do not touch and stick together.
Important Note: You do not need to be forceful, but you must be firm and precise. Quick, light touches are just annoying to the baby and do not effectively keep the wound open. A slow, deliberate stretch is much better.
What Does Normal Healing Look Like?
Parents often panic when they look into their child’s mouth a few days after the procedure. Knowing what to expect can save you a lot of anxiety.
The “White Diamond” Stage
Within the first 24 to 48 hours, the wound will develop a white or yellowish patch. This is not an infection. In the mouth, scabs do not look like the brown, crusty scabs you get on your knee. Oral tissue heals “wet,” and this white material is called fibrin. It is nature’s band-aid.
The diamond will look white, soft, and slightly recessed. This is a sign of healthy healing. If you see this, you are on the right track.
Data Point: Safety and Efficacy
It helps to know that this is a very safe path. Research has shown that serious complications from frenotomies are incredibly rare, occurring in less than 1% of cases. When you see that white patch, remind yourself that the body is doing exactly what it is supposed to do.
Week 2 and Beyond
As the weeks go on, the white patch will shrink. The diamond shape will get smaller, and new, pink tissue will fill in from the edges. By the end of the third or fourth week, the site should look fully healed, and the tissue should be pink and soft, similar to the surrounding area.
Feeding During Recovery
One of the main reasons parents seek a frenectomy is to improve feeding. However, improvement isn’t always instant. It can take time for your baby to “relearn” how to use their tongue effectively.
Breastfeeding
Some babies latch better immediately, while others struggle initially because their mouth feels different. Their tongue has a new range of motion, and they have to figure out how to control it. This is like learning to walk after having a cast removed from your leg; the muscles are free, but they might be weak or uncoordinated.
If latching is painful or difficult in the first few days, do not be discouraged. Work closely with an International Board Certified Lactation Consultant (IBCLC). They are essential partners in this journey. They can suggest different positions (like the laid-back nursing position) that use gravity to help the baby manage the flow of milk better.
Bottle Feeding
If you are bottle feeding, you might notice the baby taking in less air and spilling less milk as they heal. Use a slow-flow nipple to prevent them from getting overwhelmed as they adjust to their new sucking mechanics. Pace feeding is a great technique to use during the tongue tie release recovery period.
Data Point: Success Rates
To give you some encouragement, let’s look at the numbers. A study published in the Journal of Human Lactation found that 78% of mothers reported an immediate improvement in feeding mechanics following a frenotomy. Even if your journey takes a few days longer, the odds are heavily in your favor that things will get better.
Bodywork and Therapy
I view the release of the tongue tie as just one piece of the puzzle. The tongue is connected to the hyoid bone, which connects to muscles in the neck and shoulders. A baby who has been tongue-tied for months has likely developed tight muscles in the neck and jaw to compensate for the restriction.
This is why I strongly advocate for Craniosacral Therapy (CST) or working with a pediatric chiropractor or physical therapist who specializes in oral function. These professionals can help release the tension in the rest of the body.
Think of it this way: if you have been hunching over a computer for years, simply buying a new chair won’t fix your back pain immediately. You also need to stretch and strengthen your back muscles. The same applies to your baby. Bodywork helps integrate the new tongue mobility with the rest of the body.
Troubleshooting: When to Call the Office
While complications are rare, as your doctor, I want you to be informed. You should contact my office if you notice any of the following:
- Uncontrolled Bleeding: A small amount of spotting after stretches is normal. However, if there is active bleeding that does not stop with pressure, call us.
- Refusal to Feed: It is normal for a baby to be fussy, but they should not go prolonged periods (more than 6-8 hours) without eating. Hydration is key.
- Fever: A low-grade temperature can happen due to stress, but a fever over 101.5°F is not a typical side effect of the procedure and should be checked.
- Re-attachment: If you notice the diamond shape disappearing rapidly and the tissue looking like it is zippering shut, we may need to adjust your stretching technique.
Sleeping Patterns and Regression
It is not uncommon for sleep to be disrupted for a few nights. Your baby is processing a lot of sensory input. Their mouth feels different, and they may be sore. I advise parents to be patient during this time. Extra cuddles, contact naps, and patience are the best prescriptions.
Some parents actually report better sleep after the first week because the baby is no longer swallowing as much air (which causes gas) and is eating more efficiently (staying full longer). So, while the first few nights might be rough, there is a light at the end of the tunnel.
Emotional Support for Parents
I want to take a moment to speak directly to you, the parent. Doing stretches on a crying baby is emotionally taxing. It goes against every instinct you have to cause your child temporary discomfort. But I want to remind you that you are doing this for them, not to them.
By ensuring a proper recovery now, you are preventing potential issues down the road such as speech impediments, dental crowding, sleep apnea, and textural eating aversions. The few weeks of stretches are a small investment for a lifetime of oral health.
If you feel overwhelmed, take a deep breath. Tag-team with your partner if possible. Have one parent do the stretches while the other provides immediate comfort afterwards. You are doing a great job.
Moving Forward with Confidence
Recovery is a journey, not a sprint. Every day that you perform the wound care and support your child, you are helping them gain function that will serve them for the rest of their life. The tongue tie release recovery period is intense, but it is short.
In my practice, I see the difference this procedure makes every day. I see babies gaining weight, mothers nursing without pain, and toddlers speaking their first clear words. Keep your eye on that goal. Trust the process, trust your instincts, and remember that my team and I are here to support you every step of the way.